The Gut–Brain Axis in Child and Family Mental Health
Understand how digestion, microbes, metabolites, stress, and the brain may be connected — and how to read the science with clarity and caution.
As a pediatrician, I often hear parents say things like:
- “My child’s anxiety gets worse when their stomach is off.”
- “After antibiotics, everything changed.”
- “Stress seems to affect digestion and mood at the same time.”
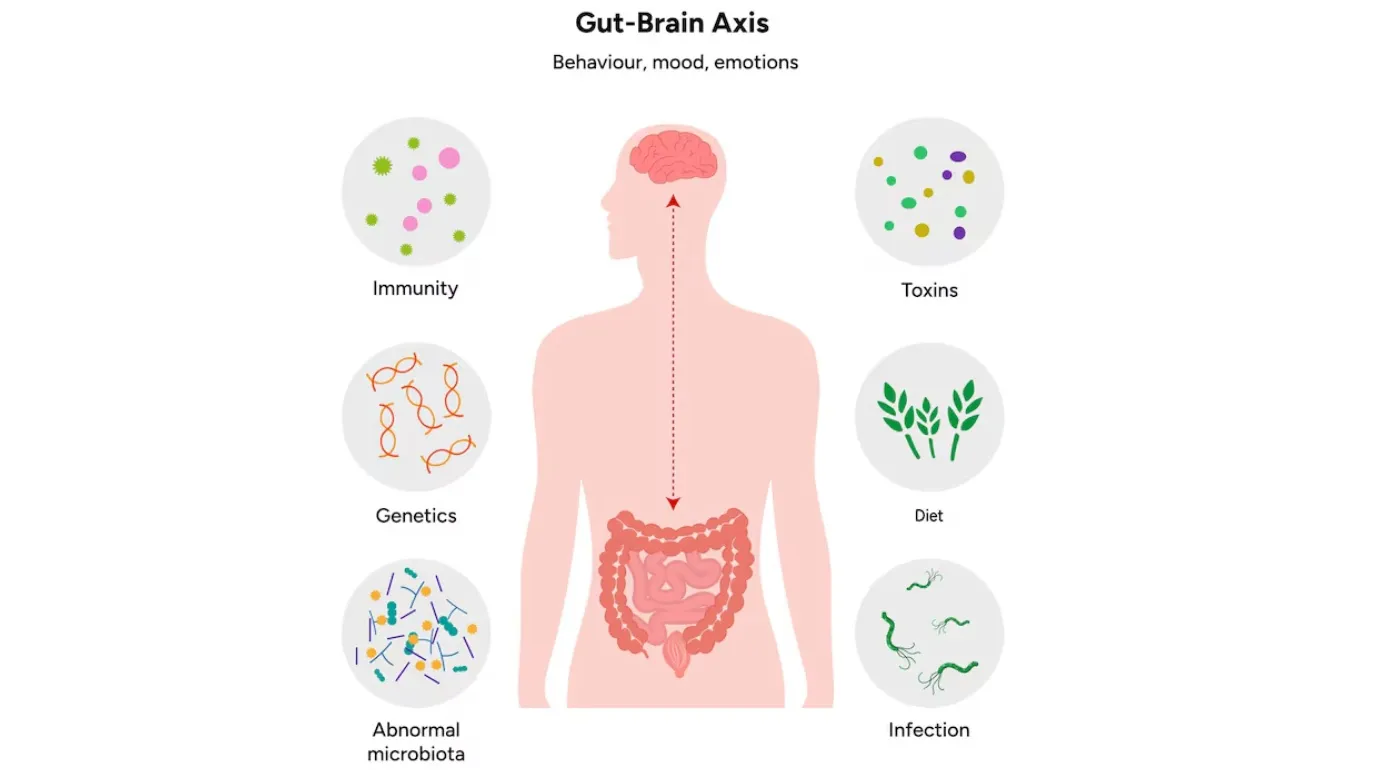
These observations are not “just in your head.” Modern research supports the idea that the gut and brain are in constant communication. This communication system is called the gut–brain axis. It includes:
- the gut microbiome
- the enteric nervous system
- the vagus nerve
- immune signals
- microbial metabolites
- hormones and stress biology
Recent reviews show that the gut–brain axis may influence mood, stress responses, behavior, cognition, and gastrointestinal symptoms, while also being influenced by diet, sleep, medications, illness, and chronic stress.
This does not mean that the microbiome is the single cause of mental health conditions, developmental differences, or autism. It does mean the gut–brain axis is an important biological system worth understanding.
Research Evidence
The 2024 Cells review focuses on how microbiome composition, metabolites, hormones, biological sex, and stress influence the gut–brain axis in mood and anxiety disorders. The 2025 Nutrients review offers a broader overview of the gut–brain axis, including the vagus nerve, enteric nervous system, neurotransmitters, short-chain fatty acids, diet, probiotics, and personalized medicine.
1. The gut and brain communicate in both directions
Signals travel from the brain to the gut and from the gut back to the brain. This communication involves nerves, hormones, immune pathways, and microbial metabolites.
2. The microbiome can influence mood and stress biology
Both reviews support the idea that gut microbes and their metabolites may shape stress reactivity, inflammation, and neurochemical signaling. The evidence is strongest for depression, anxiety, and stress-related conditions, though it is still evolving.
3. Stress can change the gut
Psychological stress may alter gut motility, permeability, immune signaling, and the composition of the microbiome. In other words, stress does not just affect the mind—it can also affect the digestive system and microbial balance.
4. Diet matters
Dietary fiber, fermented foods, and other nutrition patterns appear to influence microbial diversity and metabolite production. Both reviews discuss prebiotics, probiotics, and diet as promising but still imperfectly defined tools.
5. Human evidence is promising but mixed
The field is exciting, but both reviews emphasize major limitations:
- human microbiomes vary greatly from person to person
- many studies are small
- animal findings do not always translate to people
- it is often difficult to prove cause versus consequence
Evidence confidence
High confidence:
- the gut and brain communicate bidirectionally
- the microbiome influences immune and metabolic signaling
- stress can alter gut physiology and microbiome balance
Moderate confidence:
- microbial metabolites such as SCFAs and tryptophan metabolites influence brain-relevant pathways
- gut-targeted interventions may help some people with GI or mental health symptoms
Emerging confidence:
- personalized microbiome-guided treatment strategies
- specific probiotic strains for specific psychiatric or developmental phenotypes
- biomarker-guided precision treatment
Biological Pathway
3.1 Neural communication: the vagus nerve and enteric nervous system
The gut has its own nervous system, called the enteric nervous system (ENS), sometimes referred to as the “second brain.” The vagus nerve acts like a major communication highway between the gut and the central nervous system.
Why it matters:
- the brain can influence gut motility, secretion, and pain signaling
- the gut can influence brain activity, stress responses, and mood
3.2 Microbial metabolites
Gut microbes make biologically active compounds that travel locally and systemically.
Important examples include:
- short-chain fatty acids (butyrate, acetate, propionate)
- tryptophan metabolites
- bile acid metabolites
- phenolic compounds
Why it matters:
- SCFAs may support gut barrier function and influence inflammation
- tryptophan metabolites may affect serotonin pathways and immune signaling
- some microbial metabolites may influence blood–brain barrier integrity and brain function
3.3 Immune signaling
The gut contains a large portion of the body’s immune activity. Microbes, intestinal barrier integrity, and immune cells all influence inflammatory signaling.
Why it matters:
- gut inflammation may shape stress responses and behavior
- inflammatory cytokines may signal to the brain directly or indirectly
- the vagus nerve may help transmit some of these signals
3.4 Stress hormones and the HPA axis
Stress affects digestion, gut permeability, microbiome composition, and inflammatory activity. The hypothalamic–pituitary–adrenal (HPA) axis helps regulate stress hormones such as cortisol.
Why it matters:
- chronic stress may shift the microbiome
- the microbiome may also influence how the body responds to stress
- this may create a feedback loop between gut symptoms and emotional symptoms
3.5 Neurotransmitter and endocrine signaling
The gut and its associated cells help regulate neurotransmitters and hormones relevant to the brain.
Important molecules include:
- serotonin
- dopamine
- GABA
- norepinephrine
About 90% of the body’s serotonin is made in the gut, where it affects motility, secretion, and gut sensation, while also intersecting with broader mood-related pathways.
3.6 Nutrition and barrier integrity
Dietary fiber feeds beneficial microbes. Fermented foods may add live microorganisms. Tight junction proteins and mucus layers help maintain the intestinal barrier.
Why it matters:
- stress can weaken barrier integrity
- diet can support or disrupt microbial diversity
- barrier dysfunction may amplify immune activation
Biomarkers
Researchers are studying several categories of biomarkers relevant to the gut–brain axis.
Microbiome markers
- microbial diversity patterns
- relative abundance of specific genera or species
- stool sequencing profiles
Metabolite markers
- short-chain fatty acids (butyrate, acetate, propionate)
- tryptophan metabolites
- bile acid metabolites
- phenolic compounds such as p-cresol-like molecules in some research contexts
Inflammatory markers
- CRP
- cytokines
- markers of gut immune activation
Barrier and gut function markers
- indirect measures of permeability
- stool inflammatory markers in GI settings
- symptom-based measures of bowel function
Hormone and stress-related markers
- cortisol
- HPA-axis related measures
- stress symptom scores paired with biologic measures
Important caution: No single gut–brain biomarker can currently diagnose a mental health disorder or reliably direct treatment by itself.
Symptoms or Patterns
Parents often notice gut–brain patterns before they know the term “gut–brain axis.”
Digestive patterns
- constipation
- diarrhea
- bloating
- abdominal pain
- food-related symptom shifts
Emotional and behavioral patterns
- anxiety
- irritability
- stress sensitivity
- low mood
- sleep-related worsening of behavior
Brain–body patterns parents often report
- stress worsening stomach symptoms
- GI symptoms worsening mood or focus
- behavior changes after illness, antibiotics, or major dietary shifts
- cycles of poor sleep, poor digestion, and dysregulation
What the research supports
The reviews do not claim that the microbiome is the sole cause of depression, anxiety, autism, or other brain-based conditions. Instead, they support the idea that the gut–brain axis may contribute to symptom intensity, resilience, and variability in some individuals.
Testing or Measurement
At this stage, gut–brain axis testing is mostly used in research or selective clinical settings.
Common approaches used in studies
- stool microbiome analysis
- metabolomics
- inflammatory markers
- cortisol or stress-related measurements
- symptom questionnaires paired with biological data
What these tests can and cannot do
They may help researchers understand patterns across groups. In some clinical settings, they may help explore gastrointestinal or inflammatory contributors. But they are not yet standardized enough to serve as definitive tests for most mental health conditions.
Why testing remains difficult
- microbiomes are highly individual
- diet changes results
- timing and sample handling matter
- causation is hard to prove
- the same symptom can arise from different biological pathways
Summary for Parents
If you have noticed that your child’s digestion, mood, stress, and behavior seem connected, current science suggests you are noticing something real.
The gut–brain axis is a two-way communication system linking the digestive tract, the microbiome, the immune system, stress hormones, and the brain. Research increasingly shows that these systems can affect one another.
This does not mean that every emotional or developmental symptom starts in the gut. It also does not mean there is a single probiotic or test that will solve everything. But it does mean that gut health can be one important piece of the larger picture.
The most balanced takeaway is this:
- the gut matters
- the brain matters
- stress matters
- the relationship is real but complex
For many families, the most practical approach is to pay attention to patterns over time and work with clinicians who take both body and brain symptoms seriously.
FAQ for Parents
What is the gut–brain axis?
It is the two-way communication system between the digestive tract and the brain, involving nerves, hormones, immune pathways, and microbial metabolites.
Can the microbiome affect mood or anxiety?
Research suggests it can influence pathways related to stress, inflammation, and neurotransmitters, although it is rarely the only factor.
Can stress affect the gut?
Yes. Stress can alter motility, permeability, inflammation, and even microbiome composition.
Are probiotics proven treatments for mental health conditions?
Not in a universal way. Some strains show promise, but results vary and the science is still developing.
Should every child get microbiome testing?
Not necessarily. These tests are still evolving and are not yet stand-alone tools for most mental health questions.
References
Verma, A., Inslicht, S. S., & Bhargava, A. (2024). Gut-brain axis: Role of microbiome, metabolomics, hormones, and stress in mental health disorders. Cells, 13(17), 1436. https://doi.org/10.3390/cells13171436
Petrut, S.-M., Bragaru, A. M., Munteanu, A. E., Moldovan, A.-D., Moldovan, C.-A., & Rusu, E. (2025). Gut over mind: Exploring the powerful gut-brain axis. Nutrients, 17(5), 842. https://doi.org/10.3390/nu17050842
Latest posts

Why is p-Cresol generating buzz?
A pediatrician explains how a microbial metabolite may influence inflammation, brain function, and development.
Exciting things are coming.
Sign up to get early access!
We’re building something great – and you’ll be the first to try it.


